Translate this page into:
Barriers to Effective use of Palliative Care Services in the Acute Care Setting with Emphasis on Terminal Noncancer Diseases
Address for correspondence: Dr. Randol Kennedy, 900 O'Malley, Apartment 304, Parma, OH 44134, USA. E-mail: randolkennedy@gmail.com
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
This article was originally published by Wolters Kluwer - Medknow and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Introduction:
This study assessed the views of nurses, resident doctors, and attending physicians of the use of a readily available pain and palliative care specialty at their institution while assessing their ability to recognize terminal noncancer illnesses.
Methodology:
In community hospital consisting of an in-patient pain and palliative specialty, attending physicians, residents, and nurses participate in a survey highlighting the following: parameters for referral/consultation, definition of noncancer-related terminal illnesses, role of pain and palliative care in acute care, consult/referral delay, barriers to effective referral, recognition and withdrawal of futile care, and opioid prescription. Patterns of responses by each professional group were compared and contrasted.
Results:
The most common accepted reasons for referral were that of hospice care, terminal cancer, and uncontrolled pain, while reasons related to terminal noncancer illnesses were less accepted. A majority of approved physical and social parameters to define terminal noncancer illnesses were not universally accepted among the groups-especially among attendings and residents. While most participants agreed that the best time to refer to palliative care specialty was at the point of diagnosis of a terminal illness, >25% of participants from each group felt that referrals should be done later in the course of the illness. The most highlighted reasons expressed by attendings and residents for the delay in consult were either that of excessive withdrawal of modalities of care or interference with ongoing management that may benefit the patient. Most residents and nurses agreed that attendings' reluctance to consult is a major barrier to its utilization.
Conclusion:
Barriers to effective utilization are multifactorial, mostly relating to perceptions of the specialty as well as ineffective communication within specialties.
Keywords
Acute care
barriers to palliative care
palliative care
palliative care service
INTRODUCTION
At the institution under study, in addition to direct consult requests by a primary attending, nurses are allowed to make referrals to the onsite palliative care service. These referrals are then made into official consults after agreement by the primary attending. This method was constructed as a means to increase the number of consults; however, raw data collected by the specialty showed no improvement.
This study highlighted the possible barriers to referral to the palliative care service in an acute care hospital. Conclusions from this study will identify possible specific misperceptions of the specialty and bring the discussion to what specific factors may cause underutilization.
METHODOLOGY
A questionnaire was constructed to highlight the following:
-
Referral/consultation frequency
-
Conditions where referral/consultation is considered (based on hospital policy guidelines)
-
Conditions for referral for noncancer-related terminal illnesses
-
Opinions on the relevance of pain and palliative care in acute care
-
Reasons for consult/referral delay
-
Barriers to effective referral
-
Recognition and withdrawal of futility of care
-
Opioid use
-
Recognition of pain and palliative care as a specialty.
Internal medicine residents, nurses/nurse practitioners of medicine wards, and internal medicine primary attending physicians of a community hospital were targeted to be included in the study [Figure 1]. Those who were not residents, nurses, nurses' practitioners, or attending physicians of the above inclusion criteria were not targeted. Furthermore, nurses and attending physicians who were pain and palliative specialists were excluded from the study. For attending physicians, teaching attending physicians were targeted because of accessibility, also teaching attending physicians cover the vast majority of admissions covered in the hospital under the study (>80%).
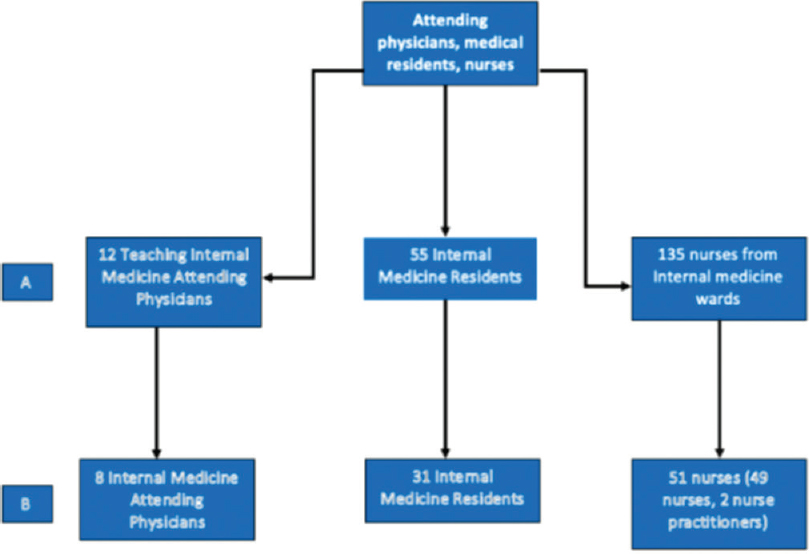
- Selection of participants
Those who were targeted were asked face-to-face if they were willing to participate and if agreed were each given one questionnaire to fill. The anonymity of responses was maintained throughout the survey – no identifiable information other than profession was required. Participants were able to fill the questionnaire at their convenience. When completed, participants either returned the questionnaires to an assigned envelope or collected by an assigned investigator.
Nurses were approached directly on the teaching internal medicine wards, the intensive care unit (ICU), and the cardiac medical unit. Residents were approached after attending a noon conference lecture in which all residents present participated in the survey. Physicians were approached directly on the wards or in their outpatient clinic. This selection process was not randomized.
Responses to each question were then tallied. Patterns of responses by each professional group were compared and contrasted, to be analyzed qualitatively. Primary points of interest assessed were that regarding palliative care, while secondary themes were that with respect to opioid prescription.
RESULTS
Forty-nine nurses, two nursing practitioners, 31 internal medicine residents, and 8 internal medicine attending physicians participated in the survey are shown in Figure 1. Those who participated were 36% of the nurses who worked on the targeted wards, 56% of the residents and 66.7% of the teaching primary attending physicians at the institution under the study.
Referrals/consults
About 89.4% of nurses reported making <4 referrals to pain and palliative specialty monthly, whereas 100% of residents placing <4 consults. This is consistent with data collected by the pain and palliative services of their monthly consults. Attending physicians reporting were less consistent, with 37.5% reported placing anywhere from 4 to 20 consults/month.
Reasons for referral/consultation
Trends in responses were relatively similar between residents, nurses, and attending physicians with the most popular reasons being that of hospice care, terminal cancer, and uncontrolled pain [Figure 2]. Less popular responses were that of nonterminal illnesses such as severe chronic obstructive pulmonary disease, chronic severe congestive heart failure, and end-stage renal disease. Patients with frequent admissions to the floor or to the ICU for burdensome chronic conditions as well as ventilated patients were the least likely to be considered for referral/consultation.
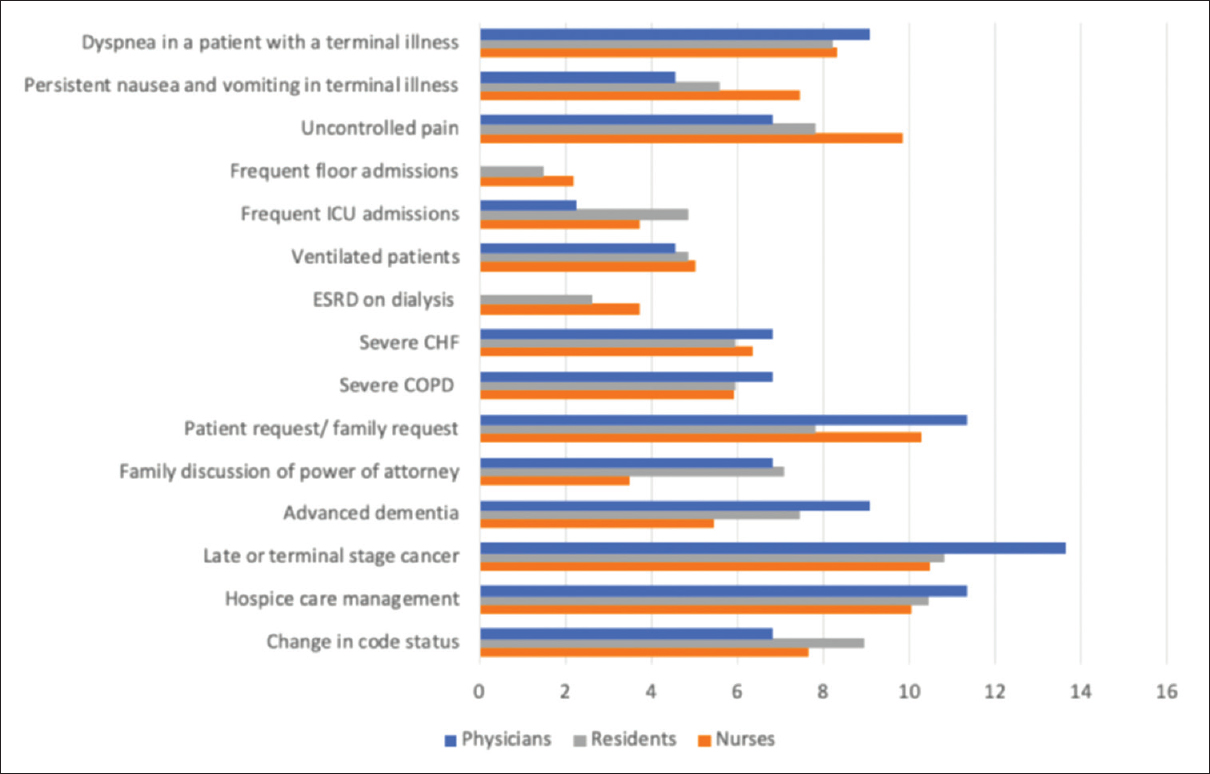
- Conditions for referral to palliative care specialty
With further exploration regarding situations where noncancer diseases were deemed adequate for referral/consultation, responses between nurses, residents, and physicians were variable. Fifty percentage of physicians and 54.6% of nurses were either uncertain or disagreeable to some degree to patients with disease-causing limiting functional capacity as candidates for consult/referral. Nearly 66.67% of residents were agreeable to some degree to these patients as candidates for consult. For diseases unresponsive to maximal pharmacological treatments, at least 60% of nurses, physicians, and residents agree to some degree these patients can be candidates for referral. Similar response rates were also for patients with advance age and bed-bound patients. For situations where treatment options less likely to be beneficial/high risk, only 58% of medical residents agreed to some degree this would adequate for palliative referral, whereas 88% of nurses and 62.5% of physicians are agreeable.
Frequent hospitalizations were not as much a convincing reason among the attending physicians compared to the other groups-64.5% residents and 66.7% nurses agreeable while only 50% of physicians agreeable to some degree. There was also a significant degree of uncertainty among the groups (22.6% residents, 20.8% nurses, and 25% physicians).
For life expectancy of 0–5 years, physicians disagreed to some degree the most frequent that this would be an adequate reason for specialist consult (37.5% of physicians, 6% of nurses, and 12.9% of residents) while nurses agreed to some degree the most frequent (84%).
Most appropriate time for palliative consult/referral
The most frequent response by physicians, residents, and nurses for the most appropriate time for consult/referral was “at the point of diagnosis of the terminal illness” (62.5% of physicians, 41.9% of residents, and 73.5% of nurses). However, 32.3% of residents responded referrals should be considered “only at patient's/surrogates request,” whereas 25% of physicians and 24.5% of nurses thought a more appropriate time would be at the point “where all interventions became futile.”
Benefit of pain and palliative specialty in acute care
About 45.2% of residents, 75% of nurses, and 50% attending physicians disagreed to some degree that “there is very little benefit of pain and palliative involvement in the acute care setting.” Of note, 37.5% attending physicians were uncertain, whereas 41.9% of residents were agreeable to some degree that there is very little benefit.
Futility of care
Majority of residents and physicians interviewed fell into the area of having some measure of comfort with futility of care (41.9% of residents somewhat comfortable and 62.5% of physicians comfortable) – however, at times (residents more so than physicians) having difficulty withdrawing futile care [Figure 3].
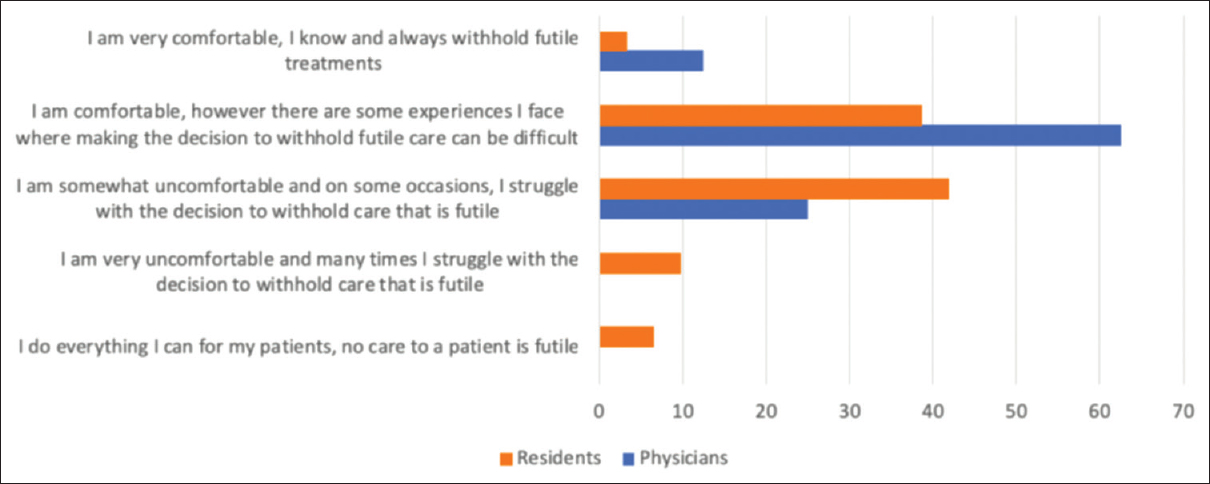
- Degrees of comfort regarding futile care
Reasons for delay in consult
Responses between physicians and residents were relatively similar [Figure 4]. The most highlighted issues were that pain and palliative services are either too aggressive in withdrawing modalities of care or that the specialty interferes with ongoing management which may benefit the patient. A significant number of attending physicians also believed that this specialty does not involve the primary team in the decision-making process. Patient's optimism about their illness was also a major concern for physicians. Most of the resident's responses mirrored that of the attending physicians, although “no reason” was the most dominant response.
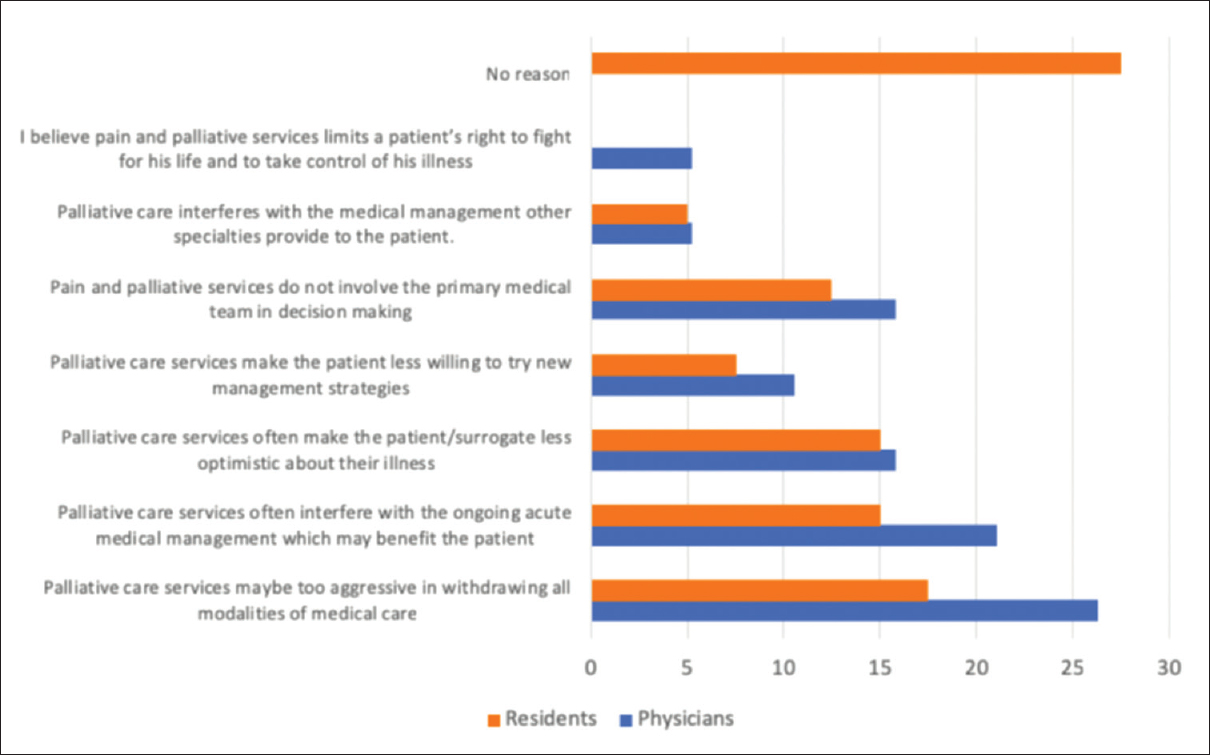
- Reasons for delay in consult
Barriers to effective service
While residents and nurses agreed that the primary attending's reluctance to consult the pain and palliative specialty is a major barrier to its effective utilization, attending physicians believe this is a less likely cause of concern [Figure 5]. Other responses were not reciprocal between the groups. For example, whereas late consultation/referral was a popular concern among the resident group, the belief that pain and palliative care means discontinuation of life-saving measures was a more popular concern for attending physicians and nurses. Patients'/relatives' lack of understanding of the specialty was also a popular concern among physicians.
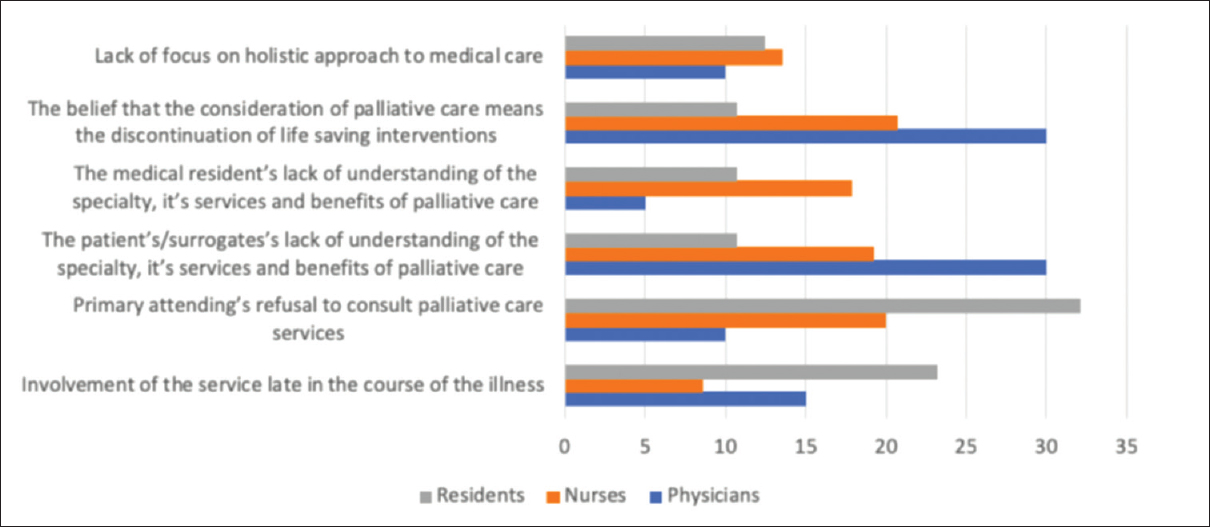
- Barriers to effective utilization of palliative care services
Opioid use
As a secondary outcome, utilization pain and palliative specialty with opioid use were also assessed. Fifty percentage of physicians stated they seldom prescribed opioids to patients, 37.5% stated they often prescribed, whereas 12.5% prescribed very often. Physician's response showed more comfort in prescribing opioids for chronic pain than in patients with terminal illness. Nearly 37.5% were somewhat comfortable, 37.5% were comfortable, and 25% were very comfortable prescribing opioids for chronic pain. About 62.5% where somewhat comfortable and 37.5% were comfortable prescribing opioids in the terminally ill patients. Fifty percentage seldom seek specialty assistance and 37.5% often seek specialty assistance when prescribing opioids. About 12.5% of physicians seek assistance very often. For residents, 35.5%, 48.4%, and 9.7% prescribe opioids seldom, often, and very often, respectively. Most resident responses were that of being somewhat comfortable with prescribing opioids for chronic pain and for terminally ill patients (48.4% for both circumstances). Being comfortable with opioid prescription in chronic pain and in terminally ill patients were stated by 25.8% and 22.6% of residents, respectively. Similar patterns to that of physicians were seen by residents regarding specialty assistance.
Whether pain and palliative assistance is warranted in patients with chronic pain had mixed responses between physicians and residents. More than 70% of residents fell into the category of “agree” to “strongly agree” (76.7%), whereas only 50% of physicians fell into those range of responses. Twenty-five percentage of physicians were uncertain and 25% disagreed. Thirteen percentage residents strongly disagreed and 6.7% disagreed.
Pain and palliative care specialty utilization and recognition
Variability of opinions among professional groups was observed. Most physicians were unsure whether the pain and palliative specialty were adequately used in the hospital (75%). Thirty-two percentage of residents disagreed that it is adequately utilized, 29% were unsure, and 22.6% agreed. Forty-four percentage of nurses disagreed, 22% were unsure, while 20% agreed.
Whereas 50% of physicians disagreed and 25% strongly disagreed to pain and palliative being a recognized subspecialty, 51% of nurses agreed and 10% strongly agreed. Residents responses were divided-36.7% disagreed, 16.7% strongly disagreed, while 30% agreed and 6.7% strongly agreed.
DISCUSSION
This project heavily highlighted short comings of addressing terminal noncancer illnesses. From the results, medical staff is more likely to consider pain and palliative specialty involvement in the management of terminal cancer than terminal noncancer illnesses. This is in keeping with the way how medical professionals perceive terminal noncancer diseases.[12] However, one can deduce that admissions, complications, and costs relating to noncancer-related illnesses far outweigh that of cancer-related illnesses.[34] Determination of whether noncancer illnesses are terminal is dependent on illness and patient-related factors;[56] however, this study showed there is marked variability among medical professionals as to what point these illnesses become terminal. Frequent hospitalization as a red flag[5] is also not appreciated among medical staff. It is in these areas of specialty underutilization that palliative care education may be most useful. Well-known specialty bodies[27] are becoming more aware of the burden nonterminal disease have on patients, as well as the lack of options to improve quality of life and longevity, and hence are emphasizing the need of adequate palliative measures during the disease course. They have also highlighted guidelines as to when palliative care can be initiated and when specialist care should be entertained. The benefits of palliative care in terminal noncancer illnesses mirror that of terminal cancer-related illnesses.[78] Therefore guidelines highlighting when to consider a palliative approach in patients with terminal non-cancer illnesses should also be emphasized as even initiation of hospice may benefit this patient population.[910] Although various guidelines have been constructed, robust objective data to accurately project mortality are limiting.[11] However, as death is often sudden and unpredictable[27] palliative measures should still be considered in this patient group.
Although most medical physicians agree that palliative specialty intervention is most beneficial at the point of diagnosis, this is not reflected practically, as most medical professionals also agree that a major barrier to effective utilization is late involvement of care. Reasons regarding this disparity may be multifactorial. Regarding futility of care, the majority of resident physicians and attending physicians have some level of discomfort determining and withdrawing futile care. This challenge was again reflected by the variability of responses regarding parameters to determine terminal cancer-related illnesses. This may be one of the reasons why physicians are reluctant to consult palliative specialties and view that the actions of the specialty in withdrawal of care may be too aggressive. A greater percentage of nurses and residents agree that attending physicians' reluctance to refer is a major barrier than physicians themselves. This highlights denial as another barrier, as previous studies support physicians reluctance to consult palliative specialty as a common occurrence.[12] This would explain why some physicians highlighted consultations of >10 patients/month, whereas raw data collected from the specialty concluded average consult rate of 0–3 patients/month.
Thoughts of palliative care being synonymous with hospice care (i.e., palliative care means withdrawing all life-saving interventions) is another misconception that limits its use.[12] This is most likely because the most frequent time the specialty intervenes is at the point when hospice care is to be implemented. Seldom, the palliative specialty is consulted earlier in the disease course where its management is less aggressive and most useful.
As perverse as this may sound, the incentives generated by the fee-for-service payment system may also be a realistic barrier (not highlighted in this study) as the implementation of palliative specialty care may inadvertently reduce revenue.[26712] This not only adds to the fear but can also lead to medical management that is not tailored to the patient's needs.
Another reason why the palliative care specialty may be perceived as too aggressive or antagonistic to the medical management is ineffective communication between the palliative specialty, the primary care team and other involving specialty teams regarding the goals of care. Perceptions pertaining to the prognosis may differ among teams and if not addressed effectively can lead to disunity in approach and ineffective communication to the patient. As a consequence, the patient/surrogate becomes confused of the goals of care, leading to dissatisfaction, false hope, delayed/prolonged bereavement, and depression. Therefore, effective communication between caregivers plays a role in effective physician-patient communication.
Opioid prescription patterns are becoming a great concern today as a result of the opioid epidemic in the US. As Ohio is one of the most affected states (based on the Centers for Disease Control and Prevention data), much discussion surrounds how best to address suboptimal practices regarding the opioid prescription. As highlighted by the study, there is some disparity between the level of comfort in prescribing opioids in patients with chronic pain and terminally ill patients, and the response to the need of pain specialty assistance. Although no conclusions can be drawn to the competence of the prescribers in managing pain, one can underscore the possible benefit of specialty intervention in situations where pain management can be challenging. Therefore, the reception to the utilization of specialty services in acute care for pain management should be addressed.
Recommendations
Possible ways in which the pain and palliative care specialty can be more frequently and effectively utilized are as follows:
-
A greater emphasis on palliative care definitions, recommendations, awareness, and utilization during residency training, which involves increase specialty rotation as well as case reports and topic discussions during morning reports and noon conferences[7]
-
A greater emphasis on palliative care definitions, recommendations, awareness, and specialty utilization to caregivers in continuing medical education training[7]
-
Caregiver teaching conferences to nurses and physicians to highlight the hospital guidelines regarding palliative care referral/consultation
-
Awareness and utilization of guidelines that guides the identification and management of various terminal noncancer diseases
-
Frequent meetings between the pain and palliative team and attending physicians highlighting ways in which communication between specialties can improve
-
Emphasizing the need of discussion between the pain and palliative team and other caregivers to address goals of care for the patient being managed, when palliative care team is consulted. These discussions may be most beneficial before communicating the goals of care to the patient
-
Implementation of ways case managers can address the role of specialty palliative care in situations where care may be deemed cost-ineffective or futile
-
Implementation of ways pain and palliative care can be involved in chronic pain, especially when strong opioids are prescribed
-
Routine course training of prescribers in pain management, opioid analgesic utilization and when to seek specialist assistance
-
Implementation of electronic medical record (EMR) protocols surrounding opioid prescription that include prompting the use of pain specialty service when strong opioids or multiple opioids are being prescribed.
Limitations
The number of participants representing each professional group (physicians, nurses, and residents) was limited by those who were willing to participate at the time. The selection of participants was not randomized; therefore, selection bias should be accounted for. The length of the questionnaire (29 questions) and the level of complexity (some questions required multiple responses were also a concern among interested candidates. The physician sample pool was also very small, and accessibility of nonteaching physicians is difficult; hence, data collection was limited to teaching physicians only. Fuirthermore, surveys were only conducted at one hospital, which may question external validity. Similar and larger studies can be constructed to address whether such conclusions can be replicated with a means to emphasize a need for general improvement.
CONCLUSION
Barriers to effected utilization are multifactorial, mostly relating to perception of the specialty as well as ineffective communication within specialties. With respect to noncancer-related illnesses, major barriers exist regarding consideration for specialty referral and definition of terminal illness. Major biases exist between that of recognition of terminal cancer-related illnesses and noncancer diseases. Pain and palliative care is not universally a recognized subspecialty, and its role in acute hospital care is underappreciated by medical professionals.
In addressing these issues, there needs to be a greater emphasis on medical professional education, physician-physician communication, and policy implementation to improve utilization and service.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Acknowledgments
We thank Dr. Katarzyna K. Hause-Wardega, MD, our mentor, who supervised the research by sharing her insight and suggestions during the development of the proposal as well as the editing of the final manuscript.
REFERENCES
- An official American thoracic society clinical policy statement: Palliative care for patients with respiratory diseases and critical illnesses. Am J Respir Crit Care Med. 2008;177:912-27.
- [Google Scholar]
- Differences in health care utilization at the end of life among patients with chronic obstructive pulmonary disease and patients with lung cancer. Arch Intern Med. 2006;166:326-31.
- [Google Scholar]
- 2017. Centers for Disease Control and Prevention. Chronic Disease – An Overview. Centers for Disease Control and Prevention; 28 June. Available from: https://www.cdc.gov/chronicdisease/overview/index.htm
- Conditions with the Largest Number of Adult Hospital Readmissions by Payer, 2011. Healthcare Cost and Utilization Project Statistical Brief #172. Agency for Healthcare Research and Quality; April. 2014
- [Google Scholar]
- Identifying patients in need of a palliative care assessment in the hospital setting: A consensus report from the center to advance palliative care. J Palliat Med. 2011;14:17-23.
- [Google Scholar]
- Palliative care and cardiovascular disease and stroke: A policy statement from the American Heart Association/American Stroke Association. Circulation. 2016;134:e198-225.
- [Google Scholar]
- Pilot study of palliative care consultation in patients with advanced heart failure referred for cardiac transplantation. J Palliat Med. 2012;15:12-5.
- [Google Scholar]
- The quality of life of hospice patients: Patient and provider perceptions. Am J Hosp Palliat Care. 2005;22:95-110.
- [Google Scholar]
- Comparing hospice and nonhospice patient survival among patients who die within a three-year window. J Pain Symptom Manage. 2007;33:238-46.
- [Google Scholar]
- Evaluation of prognostic criteria for determining hospice eligibility in patients with advanced lung, heart, or liver disease. SUPPORT investigators. Study to understand prognoses and preferences for outcomes and risks of treatments. JAMA. 1999;282:1638-45.
- [Google Scholar]
- Physician factors associated with outpatient palliative care referral. Palliat Med. 2009;23:608-15.
- [Google Scholar]






