Translate this page into:
Palliative Surgical Approach in Advanced Nonresponsive Mucinous Ovarian Cancer: A Rare Case Report
Address for correspondence: Dr. Ritesh Kumar; E-mail: riteshkr9@gmail.com
This is an open access article distributed under the terms of the Creative Commons Attribution NonCommercial ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non commercially, as long as the author is credited and the new creations are licensed under the identical terms.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Advanced mucinous ovarian cancer is a separate entity and has different biological behaviour. There is a wide range of therapeutic challenges and dilemmas in the management of these patients. The authors present a case of advanced ovarian mucinous cystadenocarcinoma with pseudomyxoma peritonei who had poor response to standard neoadjuvant chemotherapy. This case is highlighted to emphasize the challenges in the decision making for the management of advanced mucinous ovarian cancer.
Keywords
Chemotherapy
Mucinous
Ovary
Surgery
INTRODUCTION
The mainstay of any ovarian cancer therapy is a cytoreductive surgery, with optimal reduction the desirable outcome or with suboptimal reduction the achievable outcome. However, some patients presents in advanced stage, poor general condition and with mucinous histology. There is a wide range of therapeutic challenges and dilemmas in managing these patients. Here we present a case of advanced ovarian mucinous cystadenocarcinoma with pseudomyxoma peritonei who was considered to be inoperable in view of her clinical finding and computed therapy scan finding in consultation with oncologist and surgeon. However, after neoadjuvant chemotherapy, there was not a significant response. The patient subsequently underwent cytoreductive debulking surgery in a palliative approach and had significant improvement in symptoms.
CASE REPORT
A 58-year-old postmenopausal female (P9L9) patient presented to Gynae Outpatient Department with progressive distension of abdomen for 6 months. She had no bowel or bladder complains. On examination, vitals were stable, there was slight pallor, and no lymphadenopathy. On per abdominal examination, abdomen was uniformly distended, but fluid thrill was not elicited. No definite mass was palpable. On per speculum examination, the cervix and vagina were healthy. On per vaginal examination, the uterine size and adnexal mass could not be well appreciated due to tense ascites. The complete blood count, liver function test, kidney function test were within normal limit. CA125 was 28.2 U/mL. Ultrasonography (USG) showed massive ascites with large multiloculated bilateral adenexal mass. Magnetic resonance imaging abdomen showed ascites, large bilateral multiloculated adenexal mass with a large sheet of omental cake. Ascitic fluid showed mucinous malignant cells. USG guided fine-needle aspiration cytology from the ovarian mass was suggestive of mucinous adeenocarcinoma of the ovary. Upper GI endoscopy and colonoscopy were normal. Other metastatic workup was within normal limits.
Based on above findings, a diagnosis of advanced nonresectable ovarian cancer was established and collective decision made by gynecologist, oncologist and surgeon to start the patient on primary neoadjuvant chemotherapy. Patient received four cycles of systemic chemotherapy with paclitaxel and carboplatin in standard doses. However, the patient did not respond well to chemotherapy and was taken for cytoreductive surgery. Intraoperatively, approximately 5 L of thick mucinous material was removed [Figure 1]. The bilateral ovarian tumor [Figure 2] and the omental cake [Figure 3] were removed. The uterus, bladder, bowel were extensively studded and there was loss of plane between uterus and bladder, so hysterectomy was not done. Postoperatively, patient recovered well and her quality of life improved significantly. Postoperative histopathology revealed Mucinous adenocarcinoma of the ovary with metastasis to the omentum. This case is being reported to highlight the therapeutic dilemmas in the management of an advanced mucinous ovarian cancer.
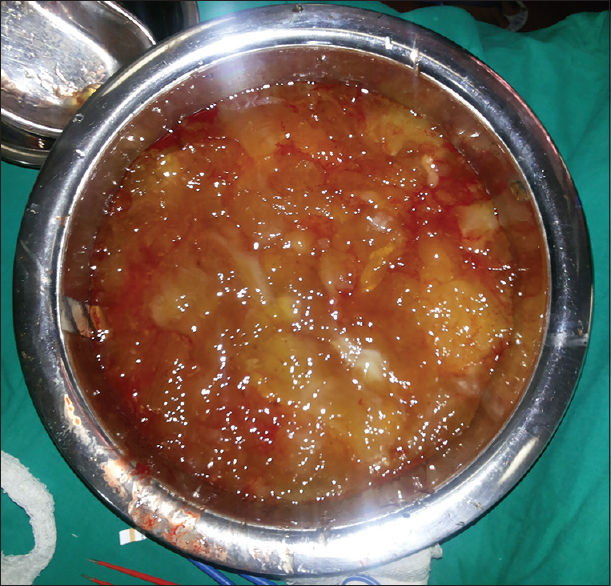
- Thick mucinous material
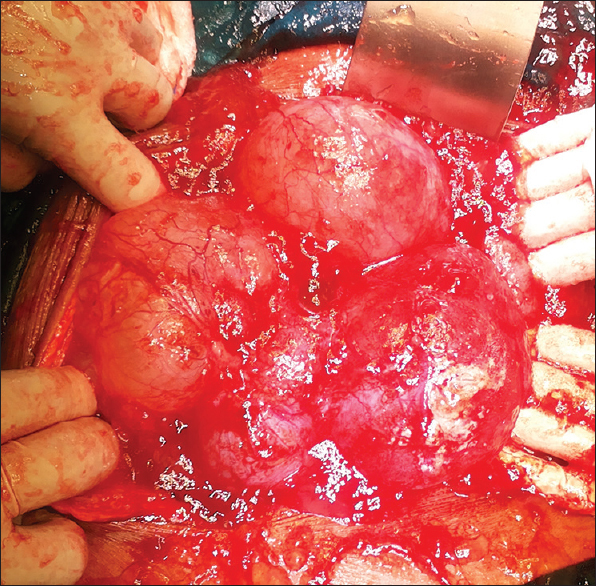
- Bilateral multiloculated ovarian tumor
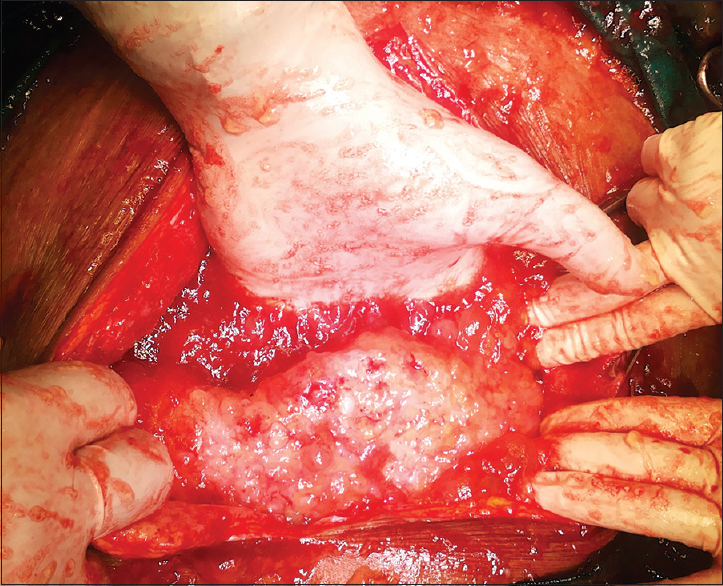
- Hard thick omental cake
DISCUSSION
Ovarian cancer is a major cause of morbidity and mortality among gynecological malignancies.[1] The standard initial treatment of patients with advanced ovarian cancer is cytoreductive surgery, followed by combination chemotherapy with paclitaxel and a platinum agent.[23] However, despite the advances in surgery and chemotherapy, the overall 5-year survival rate remains quite low. This is mainly attributed to the fact that patients usually present with advanced stage disease as well as to the lack of effective therapies.
In advanced epithelial ovarian cancer, the aim is complete cytoreduction of all macroscopic visible disease, since this has been shown to be associated with a significantly increased overall survival and progression-free survival.[4] A recent meta-analysis of more than 3000 patients evaluating the surgical outcome in ovarian cancer showed that residual tumor is a more powerful prognostic determinant than Federation of Gynecology and Obstetrics stage.[4] The timing of surgical cytoreduction in relation to chemotherapy is still debated. A large prospective trial showed that in advanced bulky stage IIIC or IV disease, three cycles of platinum-based neoadjuvant chemotherapy followed by interval debulking surgery was not inferior to primary debulking surgery followed by chemotherapy.[5] Surgical morbidity had a nonsignificant trend to be lower in the neoadjuvant arm. As a result of these data, the use of primary chemotherapy with interval surgery is becoming more widely accepted. However, the dilemma and challenge for the surgeon is that improper assessment about the operability of the case may lead to open and shut situation and cause further deterioration of the patient's condition. We faced similar dilemma for the index case while choosing for primary debulking surgery verses neoadjuvant chemotherapy and subsequently it was planned for neoadjuvant chemotherapy.
Mucinous carcinoma of the ovary accounts for 7–14% of all primary epithelial ovarian cancer.[6] However, it has been shown in a few series that advanced mucinous ovarian carcinoma has a poor outcome with a significantly worse survival.[7] The standard chemotherapy regimen used in advanced ovarian carcinoma comprises of Paclitaxel and platinum agents, but in mucinous tumors of the ovary, these agents have inferior response rates due to inherent chemoresistance.[8] This might be the reason for inferior response in the index case to neoadjuvant chemotherapy. The recent studies suggests the role of oxaliplatin and 5FU in the management of mucinous tumors of the ovary because of its biological similarity with cancer of colon.
The quality of life of the patients in advanced mucinous tumors of the ovary deteriorates with non-response to chemotherapy and gradual progression of the disease.[9] Due to poor response to chemotherapy, these patients often have distressing symptoms in form of huge abdominal distension, thick mucinous ascites not amenable to routine abdominal paracentesis, respiratory distress, constipation and decreased appetite. This leads to poor quality of life. As the thick mucinous ascites is difficult to aspirate with routine abdominal paracentesis, a thick bore needle is required for aspiration but the maximum benefit from all these distressing symptoms can be achieved from removal of mucinous ascites and maximal surgical debulking. The index case had significant relief postsurgery and her quality of life has improved significantly.
There is an increased focus on treatment of these patients with a new strategy combining maximal cytoreductive surgery with maximal regional chemotherapy (hyperthermic intraperitoneal chemotherapy, HIPEC).[10] HIPEC combines the direct effects of hyperthermia against the cancer cells with the effects of locoregional chemotherapy. Hyperthermia has been known to have direct cytotoxic effects in both temperature and time-dependent manner with a greater depth of penetration of the chemotherapy agents into the tumors. In addition, heat synergizes the cytotoxic drugs selected for intraperitoneal use at the time of surgery.
CONCLUSIONS
Advanced mucinous tumors of ovary is a separate entity and has different biological behavior and drug sensitivity. Palliatve cytoreductive surgery has a very important role in the management of these patients because of the inherent chemoresistance and poor response to standard chemotherapy. HIPEC with cytoreductive surgery is the present standard in these tumors.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Acknowledgments
Department of Pathology for histopathological diagnosis.
REFERENCES
- Advanced epithelial ovarian cancer: 1998 consensus statements. Ann Oncol. 1999;10(Suppl 1):87-92.
- [Google Scholar]
- Cyclophosphamide and cisplatin compared with paclitaxel and cisplatin in patients with stage III and stage IV ovarian cancer. N Engl J Med. 1996;334:1-6.
- [Google Scholar]
- Role of surgical outcome as prognostic factor in advanced epithelial ovarian cancer: A combined exploratory analysis of 3 prospectively randomized phase 3 multicenter trials: By the Arbeitsgemeinschaft Gynaekologische Onkologie Studiengruppe Ovarialkarzinom (AGO-OVAR) and the Groupe d'Investigateurs Nationaux Pour les Etudes des Cancers de l'Ovaire (GINECO) Cancer. 2009;115:1234-44.
- [Google Scholar]
- Neoadjuvant chemotherapy or primary surgery in stage IIIC or IV ovarian cancer. N Engl J Med. 2010;363:943-53.
- [Google Scholar]
- Mucinous epithelial ovarian cancer: A separate entity requiring specific treatment. J Clin Oncol. 2004;22:1040-4.
- [Google Scholar]
- Activity of chemotherapy in mucinous ovarian cancer with a recurrence free interval of more than 6 months: Results from the SOCRATES retrospective study. BMC Cancer. 2008;8:252.
- [Google Scholar]
- Advanced stage mucinous epithelial ovarian cancer: The Hellenic Cooperative Oncology Group experience. Gynecol Oncol. 2005;97:436-41.
- [Google Scholar]
- Quality of life in women treated with neoadjuvant chemotherapy for advanced ovarian cancer: A prospective longitudinal study. Gynecol Oncol. 2003;88:9-16.
- [Google Scholar]
- Current status and future strategies of cytoreductive surgery plus intraperitoneal hyperthermic chemotherapy for peritoneal carcinomatosis. World J Gastroenterol. 2008;14:1159-66.
- [Google Scholar]






