Translate this page into:
Symptoms in Nepali Patients with Incurable Cancers: Implications for Interventions
Address for correspondence: Dr. Richard R Love, Department of Computer Science, Marquette University, Milwaukee, WI, USA. E-mail: richardibcrf@gmail.com
-
Received: ,
Accepted: ,
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
This article was originally published by Wolters Kluwer - Medknow and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Aim:
The poor quality and limited extent of palliative care services are of concern across the globe. To identify and measure patients' symptoms in Nepal, using a cell phone questionnaire platform, the investigators conducted and previously reported a cross-sectional study of Nepali adults. The unreported details of pain and other symptoms in these study data are here considered together with possible explanations and implications for interventions to lessen these symptoms.
Methods:
In a “snapshot” cross-sectional study of patients under regular care in three tertiary care Nepalese centers, we questioned 383 patients with incurable cancers using a 15-item cell phone-validated instrument to describe their major current symptoms and their intensities. The distributions of 11 symptom-level scores and the correlations between pain and different symptom scores were determined.
Results:
Thirty-eight percent of the population (142/383) had maximal pain scores which were in the severe range, and 25% (97/383) had such scores where they were evaluated. Patients reported moderate-to-severe tiredness 48% (183/383), depression 45% (172/383), anxiety 56% (217/383), poor appetite 64% (246/383), sleep quantity 64% (246/383), and sleep quality 64% (247/383).
Conclusions:
The significant fractions of patients with severe maximal and at-evaluation pain scores suggest that inadequate recognition and treatment of such symptoms characterized care of these regularly seen patients. The high fractions of patients with mood and sleep disturbances support this reading, suggesting helplessness and hopelessness, all addressable with psychosocial, environmental, and nontoxic, inexpensive pharmacological interventions.
Keywords
Levels of pain
palliation
symptoms
INTRODUCTION
The Lancet Commission on palliative care has termed the poor state of palliative care in low- and middle-income countries a global crisis.[1] In Nepal, various domestic and international activities in palliative care, particularly educational, have been launched in the past decade.[2] In clinical practice in Nepal, currently, however, it appears that the majority of patients in need of palliative care is underserved. Affordability of care, training, access to opioids, and psychological support (at a basic level addressing abandonment) were identified critical issues in an international analysis by The Economist, and these issues are germane in Nepal.[3]
Successful palliation has to begin with detailed data on symptoms which patients with limited life expectancy have.[13] In an initial report, among 383 patients with incurable cancers, the current investigators found that half of the patients reported usual pain scores of ≥4.[4] The previously unreported detailed information on all of the 11 symptoms we assessed and their implications for management are the subject of the current communication.
METHODS
The major study goals were to determine whether symptoms data could be obtained using a cell phone questionnaire and to describe the symptoms and their intensities in patients with advanced malignancies. Briefly, after approval by scientific and ethical review boards in Nepal and the United States, we approached 383 patients with incurable malignancies presenting for care in oncology clinics at three tertiary care institutions in Kathmandu. All 383 patients provided written informed consent and agreed to provide information about their symptoms using a validated cell phone questionnaire. Further details of the acquisition of the data reported here have been published.[4] The study inclusion criteria were normal mental status, good performance status, ability to understand and cooperate with completion of the study questionnaire, and provision of written informed consent. The 15-item (11 symptoms) questionnaire covered nausea, tiredness, depression, anxiety, drowsiness, appetite, well-being, shortness of breath, and current, worst, least, and usual levels of pain in the last 24 h, constipation, quantity of sleep, and quality of sleep. Patients answered the questions by moving a cursor along Visual Analog Scale bars (0–10) to indicate intensities of each of these symptoms. The data were collected over an 18-month period that included two summers.
RESULTS
Twenty-one percent (82/383) of the patients were in the age group of 40 years or under. Details of the responses to the four pain questions showed that 37% (142/383) of the patients reported severe maximal pain levels (seven or greater), one-quarter of the patients (97/383) were in severe pain when they were being seen, and 20/383 (5%) reported pain levels of 10 at this time [Figure 1]. Fifty-nine percent (292/383) of the patients reported minimal pain levels of two or less (very mild to none). The percentages of patients reporting moderate-to-severe scores were for tiredness 48% (183/383), depression 45% (172/383), anxiety 56% (217/383), poor appetite 64% (246/383), sleep quantity 64% (246/383), and sleep quality 64% (247/383). Correlations of each of these symptoms with pain were low, ranging from 0.46 for depression to 0.28 for sleep quantity.
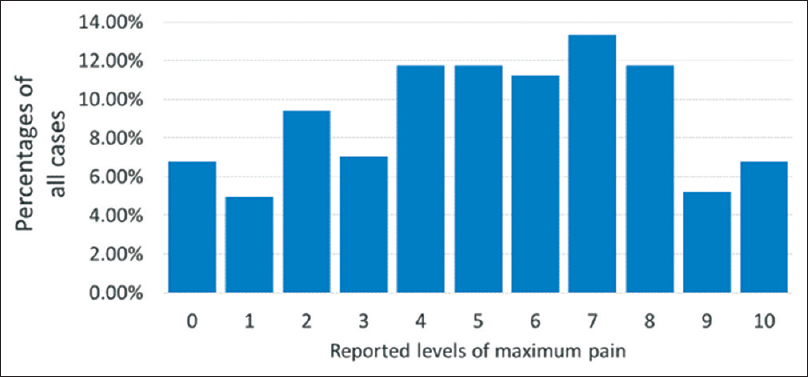
- Levels of maximum pain reported by 383 Nepali patients with incurable cancers
DISCUSSION
The age distribution of patients in this study and that of all patients in the country who develop malignancies are similar. The limitations for generalizability of the results presented in this study are that the reported-on sample of patients is first likely to be significantly less symptomatic than the majorities of patients who could not present to often distant oncology facilities because of the severities of their conditions and second a population more able to seek such specialty care because of absence of socioeconomic deprivations. Nevertheless, it is also possible that the sample here represents a sicker-than-usual group of patients.
The details of the pain picture reported here are revealing. The description in our initial report of moderate levels of pain reported in more than half of the patients provided only part of the picture needed to consider implications for more helpful clinical efforts.[4] The details now reported here seem to suggest two subgroups of patients in the sample: 59% which had minimal pain levels but 37% which suffered severe pain levels. If indeed, as believed, the majority of the patients in this study were regular patients, then there is a large fraction whose pain problem was being missed and undertreated. This is not unusual; failure to use symptom scales to assess patients' suffering is common across the world.[5]
The details of the levels of other symptoms are striking for the high fractions of mood disturbances (depression and anxiety), smaller but worrisome (15 and 19%) fractions of which were of severe levels. Poor sleep quantity and quality scores are also notable. Remarkable in these data are that correlations among pain and other symptom scores were not of significant levels at all. Nevertheless, the suggested helplessness and hopelessness in these data are all addressable with psychosocial, environmental, and nontoxic, inexpensive pharmacological interventions. Interventions addressing any of these symptoms might be expected to usefully improve functional status: the evidence is that lowering symptom scores like those for pain, by 1–2 units on such 10-point scales, does achieve such goals.[6]
How then could we bring these observations more practically to bear on clinicians' work and facilitate more impactful palliative care? In addition to those mentioned in the introduction, barriers to successful palliative management include (i) the desire of seriously ill patients to be at home and not to travel to doctors' offices or clinics; (ii) absence of “real” time (that is current) symptom type and intensity information by doctors, because symptom questionnaires are not much used at all, or repeatedly used; and (iii) absence of information on practical, affordable, and effective interventions among treating physicians and efficient systems and processes to facilitate physicians' giving successful palliative care and to lead to greater engagement of physicians broadly in this kind of care.
Specifically, how might we address these barriers? Based on the investigators' experience with the questionnaire, with a team from the Nepalese Association for Palliative Care, we are working to develop a home palliative care Nepal service (homepalliativecareNepal.net). This is a telehome palliative care system described on an informational website for patients, families, physicians, and others, with two functional parts: a cell phone patient symptom questionnaire app (as used in the study previously reported and providing the data in this communication) and a physician-service web app. On the web app, patient-submitted symptom reports can present longitudinal data by item, and the app can automatically notify the specific physician identified by the patient, through E-mail or text messaging of new reports and of major changes in, or persistently high levels of symptom scores. Further, the website app for the reports also has succinct clinical practice guidelines for palliative care and a menu of written and video patient and family interventions and educational items for physicians. In summary, this system addresses palliative care patients' desire to stay at home, provision of real-time patient symptom data to physicians, and fingertip available practical interventions with an efficient, physician-use friendly web app.
CONCLUSIONS
In a Nepali population with incurable malignancies likely to be less severely symptomatic and receiving care in tertiary care institutions, severe pain was reported in 37% of the patients. Mood disturbances – depression and anxiety – were frequent and of worrisome moderate-to-severe levels. Attention to these issues is likely to significantly improve patients' reported symptomatic and functional status.
Financial support and sponsorship
The study was financially supported by the International Breast Cancer Research Foundation.
Conflicts of interest
There are no conflicts of interest.
REFERENCES
- Alleviating the access abyss in palliative care and pain relief—an imperative of universal health coverage: The lancet commission report. Lancet. 2018;391:1391-454.
- [Google Scholar]
- Palliative care development: The Nepal model. J Pain Symptom Manage. 2007;33:573-7.
- [Google Scholar]
- Economist Intelligence Unit: The 2015 Quality of death index. London, United Kingdom: The Economist; 2015.
- symptom levels in care-seeking Bangladeshi and Nepalese adults with advanced cancer. J Glob Oncol. 2017;3:257-60.
- [Google Scholar]
- Regular use of a verbal pain scale improves the understanding of oncology inpatient pain intensity. J Clin Oncol. 1994;12:2751-5.
- [Google Scholar]
- When is cancer pain mild, moderate or severe.Grading pain severity by its interference with function? Pain. 1995;61:277-84.
- [Google Scholar]






