Translate this page into:
Bradycardia with Syncope in Carotid Sinus Syndrome: A Rare Case Report in Palliative Care
Address for correspondence: Dr. Arunangshu Ghoshal, Department of Palliative Medicine, Tata Memorial Hospital, Mumbai - 400 012, Maharashtra, India. E-mail: arun.bata@yahoo.com
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Emergencies in palliative care need to be defined by the potential distress that a clinical issue raises for a person. A 58-year-old male with carcinoma vallecula referred for palliative care presented with recurrent syncopal attacks. On examination, a swelling at the left angle of mandible pressing on the carotid sinus was detected. A clinical diagnosis of carotid sinus syndrome was made, which is an exaggerated response to carotid sinus baroreceptor stimulation and results in dizziness or syncope from transient diminished cerebral perfusion. Rapid identification and judicious interventions in time (cardiac consultation, intravenous atropine 0.5 mg, and temporary pacemaker implantation) were able to manage a potentially correctable cardiovascular emergency in his case.
Keywords
Carotid sinus syndrome
emergency
palliative care
INTRODUCTION
Palliative and supportive care is a rich and challenging area of clinical practice. Clinicians need to have a clear understanding of the life-limiting illness, the comorbid illnesses that impact so greatly on the population we serve, and the knowledge of both disease-modifying and symptomatic measures that ultimately optimize comfort and function. In patient-centered palliative and supportive care, emergencies also need to be defined by the potential distress that a clinical issue raises for that person and their family, together with the symptoms that herald this unexpected change. With the background of a life-limiting illness, many people quite reasonably interpret unexpected change as the harbinger of death. Good palliative and supportive care relies on the full range of clinical skills to deliver outcomes appropriate to a person with life-limiting illness. Through careful history, physical examination, and the judicious use of investigations, clinicians can negotiate treatment choices best tailored to a person's needs.
Here, we describe a case report of a patient having squamous cell carcinoma of vallecula. This patient was being cared by palliative care team, but rapid identification and judicious interventions in time were able to manage a potentially correctable cardiovascular emergency in his case.
CASE REPORT
A 58-year-old male presented to hospital head and neck oncology disease management group with carcinoma vallecula cT4b N3 M0.[1] A swelling in the left angle of the mandible was detected on physical examination. On magnetic resonance imaging, it was found to be encroaching the carotid space/indenting carotid arteries. Histopathological examination of an incisional biopsy revealed squamous cell carcinoma. The mass was found to be clinically/radiologically surgically unresectable, was planned for palliative intent paclitaxel-carboplatin, and referred to us for concomitant early palliative care. We formulated a comprehensive care plan for him and started him on WHO Step III analgesics[2] (tablets morphine 60 mg/day and paracetamol 2 gm/day) and pregabalin 75 mg at bedtime for neuropathic pain. While on chemotherapy, he developed Grade 4 paclitaxel hypersensitivity.[3] He was managed conservatively and started on oral metronomic chemotherapy (combination of twice daily celecoxib 200 mg and weekly methotrexate 15 mg/m2).[4] He started having syncopal attacks after a week. Chemotherapy was stopped, and he was further investigated. All fasting blood glucose, liver enzymes, serum creatinine, electrolytes (sodium, potassium, magnesium, calcium, and phosphorus), complete blood count, and electrocardiogram (ECG) were reported normal before chemotherapy. There was no history of rheumatic or cardiac disease or disorders. There was no history of cardiotoxic medication other than oral metronomic chemotherapeutic agents.
On admission, the patient had a heart rate of 48 beats/min and was hypotensive (90/70 mmHg). ECG was normal, apart from bradycardia. Renal function test and serum electrolytes (sodium, potassium, magnesium, calcium, and phosphorus) were all normal. Left ventricular structure and functions and cardiac valves were normal in echocardiography. Computed tomography scan of brain and thorax were normal; no metastatic lesions were found.
A quick cardiac consultation was done, and he was advised with intravenous atropine 0.5 mg (with instructions to repeat up to a total dose of 3 mg for bradycardia, if necessary). This helped to tide over the hemodynamic crisis. Prompt referral to a cardiologist was made. After a detailed evaluation, the cardiologist opined for temporary pacemaker implantation and to have discussions for permanent pacemaker implantation in case of persistent syncope according to guidelines from ACC/AHA/HRS.[5]
Detailed evaluation of the case pointed out the cause as left carotid sinus syndrome (CSH). It is an exaggerated response to carotid sinus baroreceptor stimulation and results in dizziness or syncope from transient diminished cerebral perfusion.[6] In this case [Figure 1], mechanical deformation of the carotid sinus (located at the bifurcation of the common carotid artery) leads to an exaggerated response with bradycardia or vasodilatation, resulting in hypotension, presyncope, or syncope. This kind of clinical features can be classified as mixed type of CSH and is seen in 20%–25% of cases.[7] To the best of our knowledge, there has been no previously published case reports in cancer palliative care on this rare syndrome.
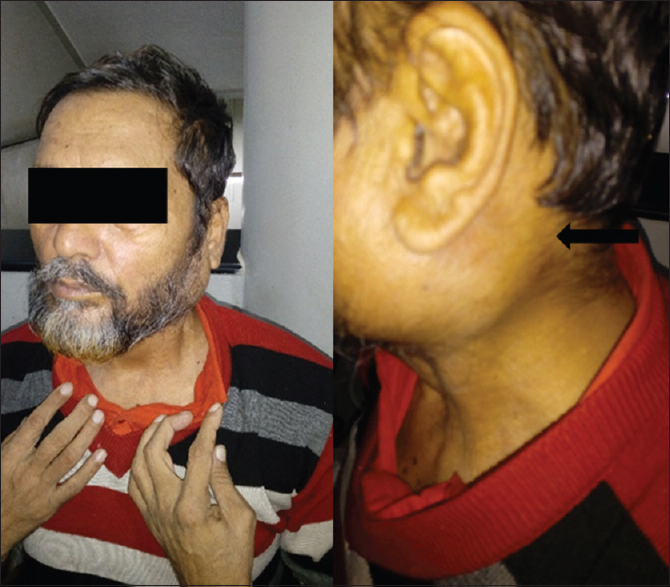
- Black arrow points to the location of the tumor on the left side of neck and pressing on the carotid sinus
DISCUSSION
In differential diagnosis of bradycardia with syncope in our patient, congenital or structural heart disease, ischemic heart disease, myocarditis, electrolyte disturbances including hypomagnesemia or hypohyperkalemia, familial atrioventricular (AV) conduction blocks, infiltrative malignancies in the heart, thyroid pathologies, and rheumatologic diseases were all excluded. The patient has no history of cardiac disease or disorders and was not administered cardiovascular medication that changes AV conduction acutely.
Development of recurrent syncope during palliative care consultation could have been fatal for this person. Prompt identification and management strongly emphasize the teaching of “correct the correctable” in palliative and supportive cancer care.[8] In Palliative Care where death is an expected outcome, emergencies are those conditions which if left untreated will seriously threaten the quality of life remaining, and prolongation of life is not usually a realistic aim. For many people with a life-limiting illness, the best symptom control remains treatment of the underlying pathology causing the new symptom. An acute deterioration in someone who is otherwise stable may become a terminal event if it is not treated. Clinically, this unexpected deterioration needs to be distinguished from the terminal stage of an advanced illness where the life-limiting illness is expected to lead rapidly to death. Such distinctions do not override individual choice where, despite a good level of function, fully informed people may choose a less active option.
CONCLUSION
Cardiovascular disorders can present as an emergency in palliative care, even in patients with no history of cardiac disease or disorders. Patients with concomitant disorders such as electrolyte disturbances, preexisting cardiovascular disorders, or those who have received cardiotoxic chemotherapy may be at an increased risk, and these cases should be monitored closely. Timely diagnosis and intervention may help us to avert sudden death and distress in patients and their families.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Acknowledgement
We would like to thank the patient and his relatives and departmental staff.
REFERENCES
- 2002. Larynx. AJCC Cancer Staging Man. New York, NY: Springer New York; :47-57. Available from: http://link.springer.com/10.1007/978-1-4757-3656-4_5
- 1986. World Health Organization. WHO's Cancer Pain Ladder for Adults. World Health Organization. Available from: http://www.who.int/cancer/palliative/painladder/en/
- Utility of risk stratification for paclitaxel hypersensitivity reactions. J Allergy Clin Immunol Pract 2017 pii: S2213-2198(17)30708-0
- [Google Scholar]
- Metronomic chemotherapy in advanced oral cancers. J Cancer Res Ther. 2012;8(Suppl 1):S106-10.
- [Google Scholar]
- ACC/AHA/HRS 2008 guidelines for device-based therapy of cardiac rhythm abnormalities: A report of the American College of Cardiology/American Heart Association task force on practice guidelines (Writing committee to revise the ACC/AHA/NASPE 2002 guideline update for implantation of cardiac pacemakers and antiarrhythmia devices): Developed in collaboration with the American Association for Thoracic Surgery and Society of Thoracic Surgeons. Circulation. 2008;117:e350-408.
- [Google Scholar]
- Carotid sinus syndrome: Progress in understanding and management. Glob Cardiol Sci Pract. 2014;2014:1-8.
- [Google Scholar]
- Dissection of carotid sinus hypersensitivity: The timing of vagal and vasodepressor effects and the effect of body position. Clin Sci (Lond). 2011;121:389-96.
- [Google Scholar]
- 2003. Introducing palliative care Fourth Edition. Radcliffe Medical Press; Available from: https://books.google.co.in/books?id=YmMwVnGTNiYC&pg=PA6&source=gbs_toc_r&cad=3#v=onepage&q&f=false






