Translate this page into:
Massive Lymphedema Necessitating Disarticulation of Shoulder Joint Following Treatment for Carcinoma Breast
Address for correspondence: Dr. Cherian Koshy, Division of Palliative Medicine, Regional Cancer Centre, Thiruvananthapuram, Kerala, India. E-mail: cherianrcc@gmail.com
This is an open access journal, and articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as appropriate credit is given and the new creations are licensed under the identical terms.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
We report a case of massive upper-limb edema necessitating disarticulation, in a cancer survivor who tended to ignore instructions regarding preventive exercises since 2002 after completion of her treatment for breast cancer. However, she was in a family situation where she was constrained to physically involve in daily chores. Consequently, she presented 14 years later with a lymphedematous arm which weighed over 31 kg, necessitating disarticulation. We highlight the role of preventive exercises in postmastectomy patients and also the efficacy of continuous nerve block techniques in preventing the development of phantom limb pain in cases of disarticulation and amputation. The role of family support for a working female cancer survivor in a country like India needs to be addressed. We salute her commitment to her family as also her grit and determination. Shoulder disarticulation was the last choice for this woman. We also want to highlight the role of the community in monitoring and preventing such disasters.
Keywords
Breast cancer
continuous peripheral nerve blockade
elastomeric pump with dual ports
massive lymphedema
shoulder disarticulation
INTRODUCTION
Lymphedema of upper limb that develops following modified radical mastectomy and adjuvant radiotherapy if left unattended can lead to various complications. Here we present such a case.
CASE REPORT
A 56-year-old female patient from Tamil Nadu presented in October 2016 with generalized weakness, vomiting, and massive lymphedema of the left upper limb. She was in distress, unable to bear the weight of her arm, and was admitted in a cot with a specially designed contraption to rest her left upper limb weighing 31 kg. She had made a similar one at home for this purpose.
Her history revealed that she had undergone modified radical mastectomy for carcinoma left breast in January 2002. Postoperatively, she underwent adjuvant chemotherapy and radiotherapy to her chest wall and axilla. She was seen in the Lymphedema Services of the Palliative Medicine Division and was taught the necessary precautions to be observed and exercises to be done. The risks involved in noncompliance were clearly communicated to her in her own language.
Since June 2002, she developed edema of the left upper arm and pain in the anterior chest wall. She was on regular follow-up and was disease free. The size of the left upper limb increased progressively by the year 2012, along with pain. The pain was a concern for which she was forced to seek medical help and did get relief from local hospital close to her home. By February 2016, her affected arm measured 120 cm in circumference at elbow region. She was offered salvage surgery by several plastic surgeons necessitating 7 to 10 sittings. She declined the suggestions and continued her life as a hard-working homemaker. Married with two children, she never received support for her work or assistance for physiotherapy, and finally she neglected it. To supplement their family income, she worked as a full-time system analyst in a transport company where a customized table was made for her affected limb to rest and she used the affected hand to type. At home, she had similar contraptions to rest her arm while sitting and when on the bed. She used to climb stairs, dress, and cook all by herself.
By October 2016, she was at her wits end, reaching the dead end of endurance, and desperately wanted to get rid of her limb, and pleaded for the same, and this was the only means to improve her quality of life. She did not have any comorbidities and was scheduled for left shoulder disarticulation.
Anesthetic management
Shifting her to the theatre was a laborious process, and it necessitated two trolleys and a “team” to coordinate the process [Figure 1]. She was given uneventful general endotracheal anesthesia and interscalene brachial plexus block under ultrasound guidance [Figure 2]. Central venous pressure (CVP) was monitored in addition to standard ASA monitoring. Intravenous fluids were given to maintain CVP between 4 and 6 cm H2O. The intraoperative period was uneventful. The upper limb was completely removed through disarticulating at the left shoulder joint and it weighed 31 kg (40% of her initial weight).
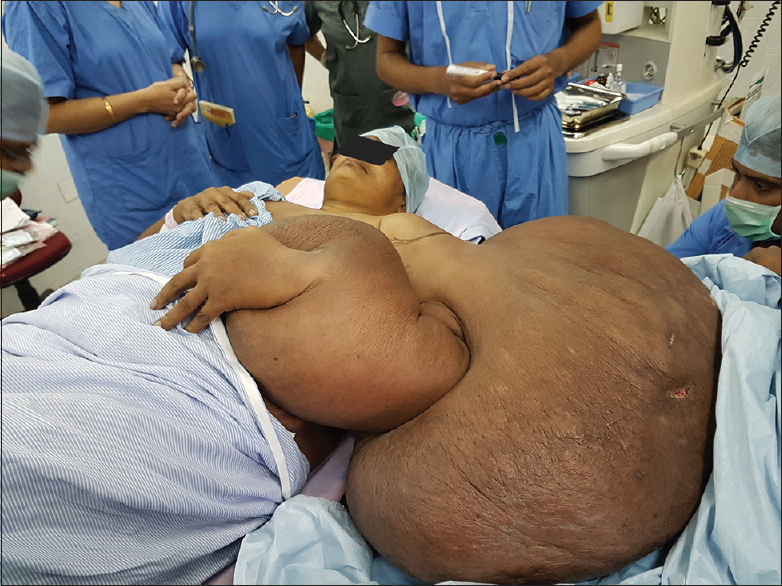
- Transferring the patient
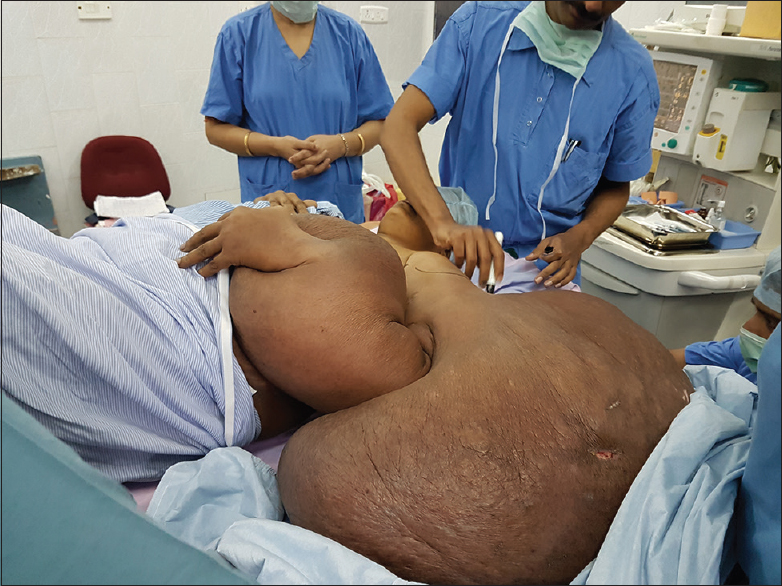
- Marking for double lumen injection port for analgesia
Postoperative analgesia was provided with a rather unique method. An elastomeric pump having a “Y-” shaped outlet tubing with two ports was used, each capable of delivering 1.04 ml/h 0.5% ropivacaine and administered to the brachial plexus (nerve sheath catheter analgesia) and the wound itself [Figure 3]. This infusion was continued for 5 days, and the patient was pain free throughout (mean numerical pain rating score 3). There was no requirement of additional analgesia. She was started on amitriptyline to preempt phantom limb pain. She was pain free and cheerful with a beaming smile during the postoperative period [Figure 4]. She was discharged on the 5th day. On follow-up 3 weeks later, the site had healed well by primary intention, with no stump or phantom pain and no phantom sensation either.
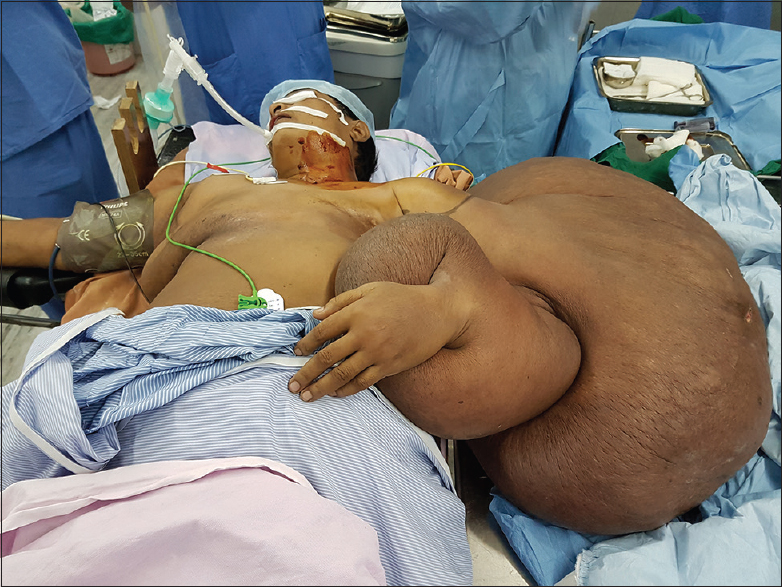
- Patient under anesthesia
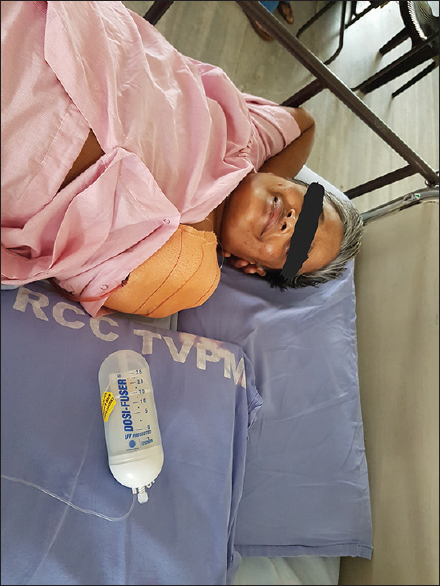
- Smiling patient following removal of lymphedematous upper limb weighing 31 kg
DISCUSSION
Breast cancer accounts for 24%–32% of all female cancers worldwide and is becoming the most common malignancies among women in India.[1] It is estimated that as many as 30%–50% patients who undergo lymph node dissection go on to develop lymphedema.[23]
Lymphedema is a poorly understood entity. It is associated with adverse physical and psychosocial consequences. It is caused by interruption of axillary lymphatic channels, by surgery and/or radiation therapy, which have a synergistic effect resulting in accumulation of protein-rich interstitial fluid in the subcutaneous tissues of the arm, decreased distensibility of tissues around joints increasing in girth of the limb and adjoining areas such as the chest wall. Although various treatment options such as complete decongestive therapy, vascularized lymph node transfer, suction-assisted lipectomy, and lymphovenous anastomosis are described, a complete cure for lymphedema is unknown. Not much evidence-based studies are available. There is good scientific evidence to support the recommendation of maintaining normal body weight or avoiding weight gain in patients who are at risk for developing lymphedema.[4] Lymphedema has a devastating and negative effect on the patient's confidence and body image. Such beleaguered patients feel that there is nothing to “feel good about” albeit being disease free, when there are restrictions on dress and social interactions.
Our patient presented with fatigue, obviously due to carrying a heavy arm. Having the “burden of baggage, fighting the battle of the bulge,” negotiating one's path tiptoeing through stigma is awful. She was a picture of a person who started with “ache going on to agony.”
There is strong scientific support for participation in a supervised exercise regimen both in patients with lymphedema and in those at risk of developing lymphedema.[4] This patient's story only exemplifies that a strong family support and religious perseverance is required to comply with such physiotherapy regimens.
When existential concerns and care of the family take precedence in a woman who has survived the assault of breast cancer, such situations happen. Empathy and an “aggressive enthusiasm” to limit lymphedema are key to prevent worsening of the situation to the extent of warranting a mutilating surgery.
Carrying such a heavy weight requires strong limb girdle muscles, and therefore, the patient gets fatigued and exhausted. Massively swollen limbs are prone to trauma and infections. Moreover, in the upright ambulant position, considerable effort is required to prevent sagging to ipsilateral side as the center of gravity shifts to the affected side. Metaphorically, the laws of Physics and Palliative Medicine seem to converge!
Our patient was in the crossroads in life's journey but had reached a dead end on presentation, craving for the disturbing disabling part of her anatomy to be removed. Phantom limb pain is a central mechanism and her mental preparation to sacrifice the limb could have helped to offset the same.
Interscalene block, nerve sheath catheter analgesia, and amitriptyline could have contributed to providing good pain relief and for avoiding unwanted acute postoperative pain and long-term pain.[567] The pathology report did not show any angiosarcomatous changes. Stewart–Treves syndrome is angiosarcomatous change that develops many years after treatment of breast cancers with lymphedema who have received radiotherapy.[8]
Elastomeric pumps are common these days. The one we used was unique in that it had a “Y-” shaped outlet, which means two ports were available and each could be connected to a separate catheter. One was connected to a catheter placed in close proximity to the severed brachial plexus,[9] while the other was placed in the wound near the cut muscles. Continuous pain relief was provided until she was ready to go home. Such pumps if available with higher flow rates could be useful in other situations such as continuous transverse abdominis plane block.
This case report underscores the importance of preventive exercises in lymphedema which could have prevented disarticulation in this patient. The efficacy of continuous regional nerve blocks in preventing the development of phantom limb pain is also another highlight.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
REFERENCES
- Statistics Breast Cancer India. Available from: http://www.breastcancerindia.net
- Lymphedema in a cohort of breast carcinoma survivors 20 years after diagnosis. Cancer. 2001;92:1368-77.
- [Google Scholar]
- Preventative measures for lymphedema: Separating fact from fiction. J Am Coll Surg. 2011;213:543-51.
- [Google Scholar]
- Postoperative orthopaedic pain – The effect of opiate premedication and local anaesthetic blocks. Pain. 1988;33:291-5.
- [Google Scholar]
- Postoperative pain after inguinal herniorrhaphy with different types of anesthesia. Anesth Analg. 1990;70:29-35.
- [Google Scholar]
- Phantom limb pain in amputees during the first 12 months following limb amputation, after preoperative lumbar epidural blockade. Pain. 1988;33:297-301.
- [Google Scholar]
- Nerve sheath catheter analgesia for forequarter amputation in paediatric oncology patients. Anaesth Intensive Care. 2013;41:671-7.
- [Google Scholar]






