Translate this page into:
Gabapentin for Chronic Refractory Cancer Cough
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.
This article was originally published by Medknow Publications & Media Pvt Ltd and was migrated to Scientific Scholar after the change of Publisher.
Abstract
Vagal sensory neuropathy or vagal hypersensitivity has been implicated in the pathophysiology of chronic cough. Earlier reports have shown gabapentin to be effective in sensory laryngeal neuropathy and symptom conditions that have a proven neural origin. We present a case report of a patient with chronic refractory cough due to a soft tissue mass in the lung that caused compression of the mediastinal structures. The patient was successfully treated with gabapentin with reduction in the cough intensity, duration, and frequency.
Keywords
Cancer
Gabapentin
Refractory cough
INTRODUCTION
Cough is one of the most distressing symptoms in cancer patients with lung or mediastinal metastasis or due to complications of cancer treatment.[1] Twenty to 42% of cough do not respond to conventional medications and are referred to as refractory cough and these are often a medical challenge.[2] Refractory cough is known to have central sensitization mechanism such as neuropathic pain. It shows features such as abnormal throat sensation (laryngeal parasthesia), increased cough sensitivity to tussigens (hypertussia), and cough triggered by nontussive stimuli such as cold or talking (allotusia).[3] Gabapentin is known to be effective in treating neuropathic pain with central sensitization and findings from the present case predicts its effectiveness in treating refractory cancer related cough. It further affirms the fact that vagal neuropathy may be associated with refractory chronic cough.
CASE REPORT
A 15-year-old boy, who had previously been diagnosed with malignant spindle cell sarcoma, was referred to the Department of Palliative Care and Psycho-oncology for chronic refractory cough. Following histopathological diagnosis of spindle cell sarcoma of right lower limb in the year 2014, he had undergone surgery followed by radiotherapy for local control. In May 2015, he presented to the Clinical Oncology Department with a history of persistent dry cough of 6 months duration. A computed tomography scan of thorax [Figure 1] revealed a large heterogenous hypodense soft tissue mass (10.5 cm × 10.3 cm) in the right lower lobe with extension to the left atrium through the right inferior pulmonary vein. In addition, there were enlarged right paratracheal, subcarinal, and hilar lymph nodes.
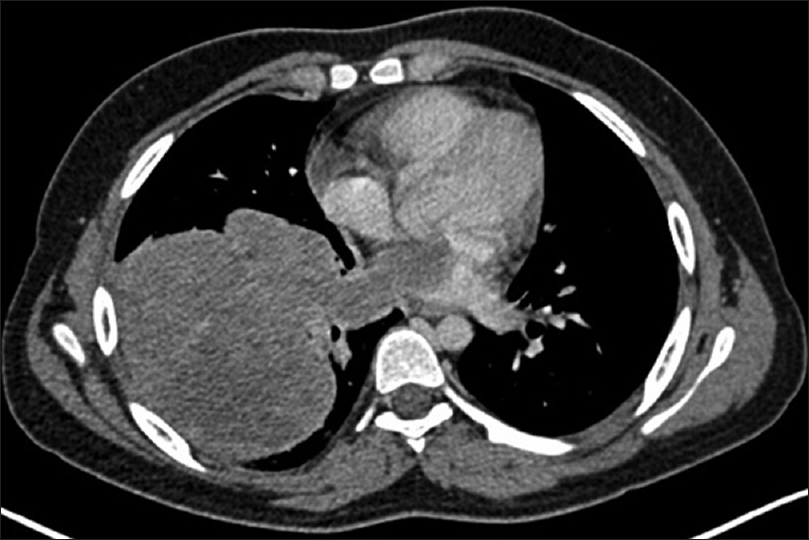
- Computed tomography scan of thorax showing the mass in the right lower lobe with extension to the left atrium through the inferior pulmonary vein
The child had persistent cough for the duration of 6 months. The cough intensity on a numerical rating scale (NRS) was 10 (out of 10). Each bout of cough lasted for 30 s and there were 20 such bouts in a day. Cough was severe in the morning and was triggered by activities that involved walking, talking, or exposure to the cold environment. The Leicester cough score[4] was 7.5. His Eastern Cooperative Oncology Group (ECOG) performance status score[5] at the time of presentation was 3. A trial of codeine phosphate started by the primary treating team did not reduce cough but instead caused excessive drowsiness and giddiness due to which he had to stop the medicines.
Patient was started on gabapentin 50 mg 3 times a day and advised to increase the dose by 50 mg every 3 days until response was obtained or the child felt drowsy (in the latter case, the drug dose would be decreased). The patient responded significantly well with 200 mg/day of gabapentin after 1 week without any side effects such as drowsiness or giddiness and he continues to improve. There was a decrease in the cough intensity to 2 (out of 10 on NRS) and both cough duration and bouts (2/day). The ECOG performance status improved to 1. The Leicester cough score improved to 18.8. The child is now able to enjoy his routine life and socialize with friends and relatives.
DISCUSSION
Patients with primary or metastatic cancer of the lung often present with distressing symptoms such as breathlessness and cough which significantly impacts their quality of life. There are multimodal options for treatment in cancer related cough which include corticosteroids, bronchodilators, brachytherapy, laser therapies, and opioids. Our patient had an extensive mass crossing the mediastinum which precluded radiation to the mass as this involved significant risk to the mediastinal structures. Opioids are commonly used in cancer patients for the management of pain, cough, and breathlessness. Opioids act by stimulating the mu receptors in the cough centers of the brain and helps in suppressing the cough. In one study, slow release morphine sulfate showed a significant improvement in the cough related quality of life as compared to placebo and this was not associated with cough reflex sensitivity which is consistent with central action of morphine.[6] However, our patient was given a trial of codeine with no response. The treatment, on the contrary, caused significant drowsiness and giddiness affecting his quality of life.
Cough reflex is mediated by the stimulation of the vagal primary afferent nerve distributed along the tracheobronchial tree.[7] Thus, rapidly adapting receptors of the vagal afferents are known to be evoked by mechanical stimuli and deformity in the airway epithelium, which results in cough.[8] Thus, an unresectable mass in the mediastinum acts as a constant source of irritation for the airway which in turn triggers cough. Neuromodulatory agents such as gabapentin have shown promising results in relieving sensory neuropathic cough. We used gabapentin in our patient with successful control in cough intensity, duration, and frequency. Gabapentin is a lipophilic structural analog of the neurotransmitter gamma aminobutyric acid which is proven to have a central action. It is known to act on the alpha 2 and delta receptor of calcium channel inhibiting the release of neurotransmitters such as substance P, a tussigenic agent, and possibly inhibits the N-methyl-D-aspartate receptors.[9]
Recent trials have shown the superiority of gabapentin in reducing the frequency and intensity of cough.[101112] Peripheral cough sensitivity to capsaicin was not changed by gabapentin which proves its central effect.[11] In the same study, there was a significant improvement in cough related quality of life in the gabapentin arm.[11] The common side effects of gabapentin include dizziness, fatigue, headache, and confusion which was not reported by our patient.[11]
CONCLUSION
Sensory neuropathic cough is emerging as a distinct clinical entity. Gabapentin has been shown to successfully treat chronic refractory cough as in this case. There is, thus, a need to explore the use of neuromodulatory agents in symptom conditions which are known to have a neural origin such as cough, pruritus, and hiccoughs.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
REFERENCES
- Unexplained (idiopathic) cough: ACCP evidence-based clinical practice guidelines. Chest. 2006;129:220S-1S.
- [Google Scholar]
- Chronic refractory cough as a sensory neuropathy: Evidence from a reinterpretation of cough triggers. J Voice. 2011;25:596-601.
- [Google Scholar]
- Development of a symptom specific health status measure for patients with chronic cough: Leicester Cough Questionnaire (LCQ) Thorax. 2003;58:339-43.
- [Google Scholar]
- Toxicity and response criteria of the Eastern Cooperative Oncology Group. Am J Clin Oncol. 1982;5:649-55.
- [Google Scholar]
- Arnold's nerve cough reflex: Evidence for chronic cough as a sensory vagal neuropathy. J Thorac Dis. 2014;6:S748-52.
- [Google Scholar]
- The clinical and pathophysiological challenge of cough. In: Chung KF, Widdicombe JG, Boushey HA, eds. Cough: Causes, Mechanisms and Therapy. 2003. p. :3-10.
- [Google Scholar]
- Analgesic action of gabapentin on chronic pain in the masticatory muscles: A randomized controlled trial. Pain. 2007;127:151-60.
- [Google Scholar]
- Chronic cough as a sign of laryngeal sensory neuropathy: Diagnosis and treatment. Ann Otol Rhinol Laryngol. 2005;114:253-7.
- [Google Scholar]
- Gabapentin for refractory chronic cough: A randomised, double-blind, placebo-controlled trial. Lancet. 2012;380:1583-9.
- [Google Scholar]
- Gabapentin in the treatment of intractable idiopathic chronic cough: Case reports. Am J Med. 2006;119:e13-5.
- [Google Scholar]






